Rediscover radiant health with Baromedical Associates LLC’s hyperbaric therapy for radiation damage after cancer treatments. Our specialized services offer a transformative approach to address the unique challenges of radiation-induced tissue damage.
With a team of certified technicians and multi-disciplinary physicians, we are committed to revitalizing your well-being in a serene and private environment. Say goodbye to limitations and embrace a future of renewed vitality.
Take the first step towards rejuvenation and healing by scheduling your consultation with a Baromedical Associates clinic today.
Delayed radiation injury refers to the long-term effects that can occur months or even years after receiving radiation therapy for cancer treatment. While radiation therapy effectively targets and kills cancer cells, it can also affect nearby healthy tissues. Delayed radiation injury typically manifests as damage to the irradiated area’s blood vessels, connective tissues, and organs.
Common symptoms may include chronic pain, fibrosis (thickening and scarring of tissues), impaired wound healing, skin changes, and dysfunction of affected organs. The severity and onset of delayed radiation injury can vary among individuals, and proper management and monitoring are crucial to mitigate its impact on a patient’s quality of life.
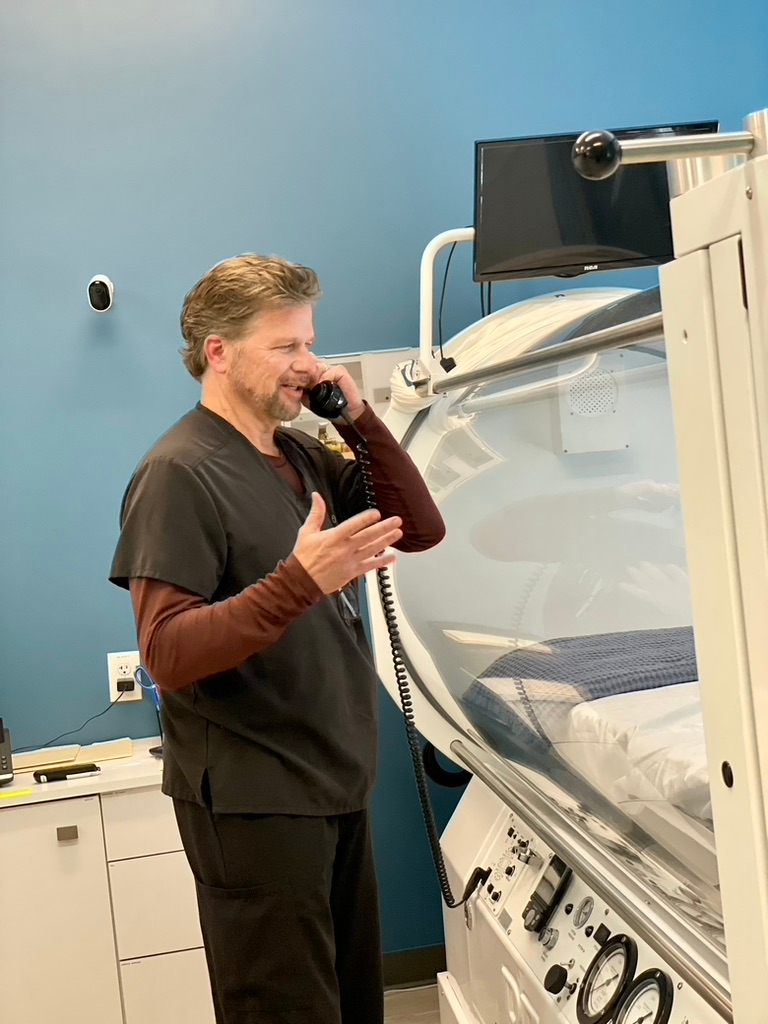
Though radiation therapy effectively targets cancer cells, it can inadvertently harm nearby healthy tissues by limiting blood flow and oxygen supply. With HBOT for radiation damage, patients breathe 100% pure oxygen while in a pressurized chamber which allows oxygen to dissolve in the bloodstream at higher levels.
This increased oxygen delivery promotes tissue healing and regeneration, enhances the formation of new blood vessels, and reduces inflammation. HBOT for radiation tissue damage can alleviate radiation-induced tissue damage, improve wound healing, reduce pain, and enhance the overall quality of life for individuals affected by radiation damage.
HBOT offers several benefits for individuals with radiation damage. The most common advantages include:
HBOT for radiation damage is administered in a specialized hyperbaric chamber. The patient enters the chamber and breathes 100% pure oxygen at increased atmospheric pressure, allowing a higher oxygen concentration to dissolve in the bloodstream.
The treatment is carefully monitored and supervised by trained medical professionals. A series of sessions is typically recommended, each lasting approximately 90 minutes. The number of sessions and treatment duration may vary depending on the severity of the radiation damage and individual patient needs. During the session, patients can rest comfortably in the chamber and may choose to listen to music, watch TV, or simply relax.
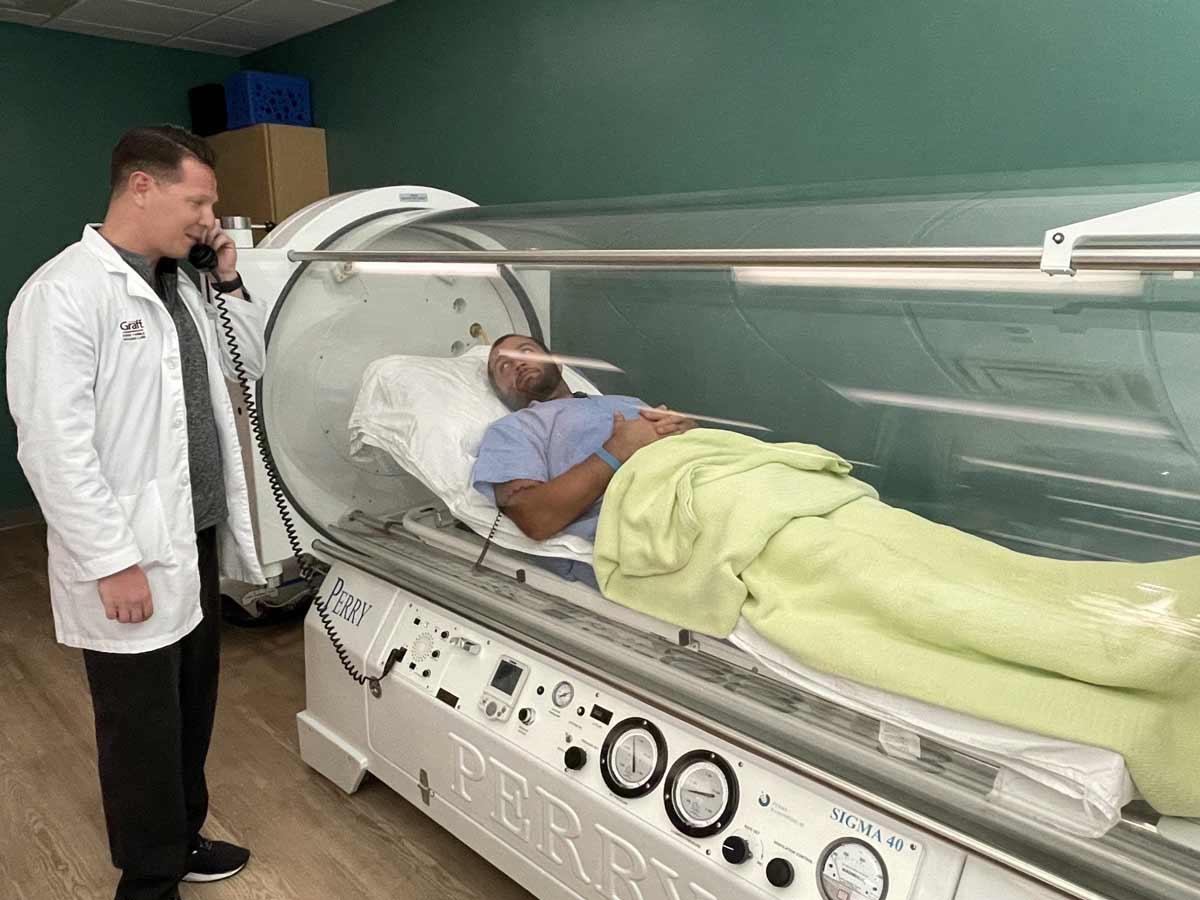
At Baromedical Associates, our dedicated team of certified technicians and multi-disciplinary physicians is committed to helping you regain your vitality and well-being.
Experience the transformative power of Hyperbaric Therapy as we address the unique challenges of radiation-induced tissue damage. Say goodbye to limitations and embrace a future of renewed health.
Take the first step towards your healing journey by scheduling your consultation with Baromedical Associates today.